McKeown Medical
167 Bath Street, Glasgow, G2 4SQ
Date posted — 18.12.25
When you’re trying to conceive, it’s natural to focus on your ovulation cycles, hormone levels, and lifestyle habits. However, one often-overlooked cause of fertility challenges is the presence of uterine polyps. These small growths in the womb may be benign, but they can significantly impact your chances of getting pregnant.
At McKeown Medical, we understand how frustrating fertility issues can be. This article will help you understand what uterine polyps are, how they might affect your fertility, how they’re diagnosed, and what treatment options are available.
Uterine polyps (also known as endometrial polyps) are small, soft growths that develop in the lining of the uterus. They are made up of the same tissue as the uterine lining, but grow in a way that protrudes into the uterine cavity. While most are benign (non-cancerous), they can vary in size from a few millimetres to several centimetres and may occur singly or in clusters.
There are two main types:
How common are they?
Uterine polyps are relatively common, particularly in women aged 30 to 50, and especially those experiencing hormonal fluctuations. It’s estimated that around 10%–24% of women in this age group may develop them.
Symptoms to watch out for include:
In many cases, however, polyps may cause no symptoms at all and are only discovered during fertility investigations or routine scans.
What causes them?
The exact cause isn’t always clear, but uterine polyps are linked to hormonal imbalances, particularly excess oestrogen. Factors such as obesity, age, and the use of certain medications (such as tamoxifen) may also increase your risk.
So, how exactly do uterine polyps affect fertility?
These growths can interfere with your ability to conceive in several ways:
Blocking embryo implantation
Polyps that occupy the uterine cavity can disrupt the environment where an embryo would normally implant and develop. Even small polyps in key locations may reduce the chances of successful implantation.
Obstructing sperm transport
Depending on their size and position, polyps can physically interfere with the passage of sperm through the uterus, reducing the likelihood of fertilisation.
Triggering inflammation
Polyps may cause subtle, chronic inflammation in the uterus, which can create a less hospitable environment for embryo development.
Not all polyps pose a threat to fertility, but those that are large, multiple, or located near the uterine fundus (top portion of the uterus, where implantation often occurs) are more likely to be problematic.
It’s important to note that while there’s a clear association between polyps and infertility, this doesn’t mean every polyp causes infertility. However, removing polyps, especially in women undergoing fertility treatments like IVF, has been shown to improve pregnancy rates significantly.
If you’re experiencing symptoms or struggling to conceive, it may be worth investigating whether polyps could be a factor.
Diagnosis options include:
Routine pelvic exams or abdominal ultrasounds are unlikely to detect uterine polyps effectively, especially if they are small or asymptomatic.
The good news is that uterine polyps can be effectively treated, often with minimal downtime and excellent outcomes for fertility.
Common treatment options include:
Hormonal treatments
Medications like progestins or GnRH agonists may temporarily reduce polyp size, but are generally less effective for long-term management and are not typically recommended when fertility is a concern.
Hysteroscopic polypectomy
This is the most definitive treatment. It allows for precise removal of polyps under direct visualisation, often in a day-case setting. Recovery is generally quick, with most women returning to normal activities within a few days.
Offered at McKeown Medical, this minimally invasive technique removes polyps while preserving the surrounding uterine tissue. It’s particularly useful for women planning to conceive, as it maintains uterine integrity.
What to expect after treatment:
Uterine polyps are a common but often overlooked cause of infertility. Fortunately, with the right diagnosis and expert treatment, most women can go on to conceive successfully.
At McKeown Medical, we specialise in women’s health and fertility, offering state-of-the-art diagnostics and advanced treatments including hysteroscopy scans and MyoSure® care, led by our experienced consultant gynaecologist, Dr Iain Martin.
Whether you’re actively trying to conceive, undergoing fertility treatment, or simply want peace of mind, we’re here to help.
Book a health consultation today to get started on your journey to better gynaecological health.

Discover what ‘True Skin Age’ means, how it’s measured using VISIA, and the evidence-based ways to improve your biological skin...
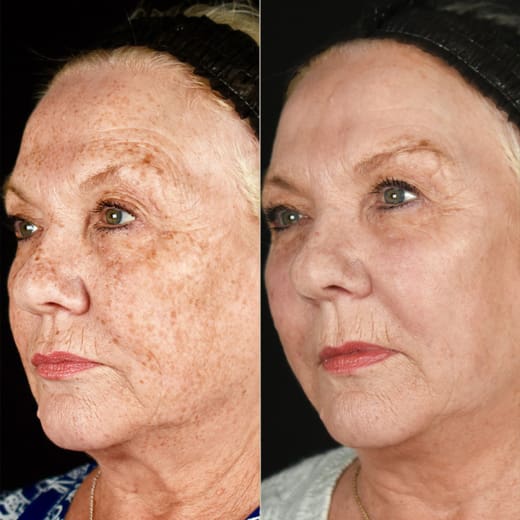
Pigmentation, redness and texture issues all have different causes. Learn what’s happening beneath the skin, and why VISIA analysis helps...

Skin quality is the missing piece in aesthetic medicine. Discover why tone, texture and clarity matter—and how lasers and VISIA...
1 / 3
2 / 3
3 / 3

Discover what ‘True Skin Age’ means, how it’s measured using VISIA, and the evidence-based ways to improve your biological skin...

Pigmentation, redness and texture issues all have different causes. Learn what’s happening beneath the skin, and why VISIA analysis helps...

Skin quality is the missing piece in aesthetic medicine. Discover why tone, texture and clarity matter—and how lasers and VISIA...
Here’s another gorgeous upper blepharoplasty result from our phenomenal surgeon, @bramhallplasticsurgery.
This patient is 62 years old and came to us for upper eyelid surgery just 2.5 months ago. Russell performed the procedure while she was awake with just a few numbing injections. Here at the clinic we can offer facial surgery with local anaesthetic for those who want to remain awake, or with deep sedation for anyone who’d prefer to sleep throughout (without the downsides of general anaesthetic!)
Thank you to this patient for allowing us to share her fabulous result - her scars are already settling beautifully and will continue to fade over the next 12 months.
What do you think?

Our resident superstar breast surgery expert Dr Kavita was asked to talk about trends in breast surgery on BBC Radio Scotland today. This was Kavita’s first ever live interview and we thought she nailed it!
What do you think?

And this is why combination treatments always win!
This lovely patient is in her 50s and was noticing all of the classic signs of ageing. She was starting to see some jowls forming, the neck was becoming more saggy and she felt she was looking tired.
At this stage in the ageing process it is not one thing that is responsible for causing the tired expression, its a combination of changes that are working together which is why we need a combination of treatments to target it effectively.
We did some sofwave treatment first to tighten the skin on the face and neck. Sofwave is very effective at tightening the skin, but remember: the skin is only the outer layer of the face, so we supported the treatment with some volume replacement in the deeper layers.
I decided to post her selfie style before and afters as well as her clinical pictures so you can see how it looks in real life, as well as the clinical up-close detail. The patient is over the moon with her results.
What do you think?

Here is another beautifully balanced deep plane face and neck lift by the skilful @bramhallplasticsurgery.
The deep plane technique, as the name suggests, works at a deeper level, repositioning the underlying structures of the face and neck rather than simply tightening the skin. By addressing the deeper tissues, we can restore more natural proportions, refine the jawline, and create a smoother, more defined contour beneath the chin - especially when the patient moves or bends their neck forward.
To achieve this impressive improvement in the neck, even in flexion, Russell reduced the deep fat (from under the muscle), trimmed and shaped the salivary glands and reconstructed the muscles of the neck to create a rejuvenated result. This is a much more sophisticated procedure compared with a standard face and neck lift.
At just 2 months post-op, her result is already beautifully balanced. The jawline is sharper, the neck more sculpted, and everything sits in harmony with the rest of her features. Scars are settling well and will continue to soften over time.
She may choose to refine things further with laser resurfacing for skin quality and subtle volume restoration in the mid-face, but even at this stage, the transformation speaks for itself.
Thank you to our patient for allowing us to share her journey.
What do you think?

Thank you to this lovely patient for allowing us to share her beautiful result from the talented @bramhallplasticsurgery.
This patient is just 2.5 months after upper eyelid surgery, and already looking incredibly fresh and natural. The scars are settling very well and will continue to soften over the coming months.
The incisions are carefully placed within the natural eyelid crease, making them very difficult to see once healed. Excess skin has been removed to open up the eye area, while maintaining a soft, natural appearance.
A small amount of muscle was reduced at the outer part of the eyelid to address hooding, without affecting the central area. This helps preserve a youthful fullness above the eye. There has also been a conservative reduction of the lateral brow fat to further refine the contour. This highly tailored, bespoke approach to surgery is the attention to detail that lies at the heart of our clinic’s approach and philosophy.
As with many patients, her anatomy meant these changes developed earlier than expected. In the right cases, surgery at a younger age can deliver a subtle but very impactful improvement.
What do you think?

Happy Easter from our excited little bunnies 🐣🐰

Thank you to our lovely patient for allowing us to share these photos.
This is just 4 weeks after her first session (of three) with Juläine and we’re already starting to see a soft return of fullness and improvement in skin quality.
Juläine is not a traditional filler. It works by stimulating your body’s own collagen production, gradually restoring structure, firmness and elasticity from within.
This is just the beginning. As collagen continues to rebuild over the coming weeks and months, results will become more noticeable with improved support, smoother contours and a natural, refreshed appearance.
The patient is delighted with her progress so far. What do you think?

And this is why HA fillers have never gone out of fashion in our practice!
This lovely patient had all the classic signs of volume loss in her face and there is no other non-surgical treatment that can address this quite as quickly, effectively and non-invasively as HA filler. Of course, it needs to be carefully and sensitively applied.
This patient had a total of 10mls of HA as well as some wrinkle relaxing on the upper face. She is delighted with her restoration. What do you think?

Upper eyelid surgery isn’t just for ageing eyes! Some patients naturally have excess upper eyelid skin from a young age due to their anatomy, like this 29-year-old patient who had a congenital upper eyelid fold and recently underwent an upper blepharoplasty with the ever-talented @bramhallplasticsurgery.
The excess eyelid skin rested directly on her eyelashes, causing irritation and a persistent feeling of heaviness around the eyes which had been bothering her for several years. Upper eyelid surgery can address both functional symptoms and aesthetic concerns, helping patients achieve a lighter, more open eye appearance.
This patient is just 7 weeks after surgery. At this early stage of healing the scars are still maturing and in younger patients this process can take slightly longer. The incision is placed within the natural eyelid crease and as healing progresses the scar typically fades and becomes extremely difficult to see, often blending into the natural eyelid fold.
She`s delighted with the results so far, and we`re grateful to her for allowing us to share her results with you.
What do you think?
